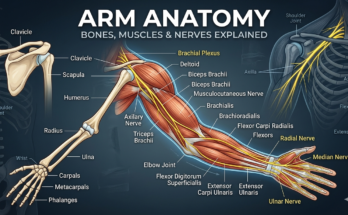
What the Anti Inflammation Diet Actually Is And How to Start It This Week
Your doctor used the phrase. Maybe it came up during bloodwork, after a joint pain complaint, or mid conversation about your cholesterol. Now you’re here, staring at a term “anti inflammation diet” that sounds medically significant but not exactly actionable.
Here’s the thing: there isn’t one certified program you sign up for. No rulebook, no label on a box. It’s an eating direction a consistent set of choices that keeps your immune system from staying on low grade alert indefinitely. The good news is that the direction is clear, and you don’t need to overhaul your kitchen overnight.
This guide covers the anti inflammation diet for generally healthy adults managing chronic low grade inflammation. It does NOT address autoimmune conditions lupus, Crohn’s, rheumatoid arthritis where a doctor supervised protocol is required.
What Is an Anti Inflammation Diet?
An anti inflammation diet is an eating pattern that prioritizes whole, minimally processed foods shown to reduce chronic systemic inflammation while consistently limiting refined carbohydrates, added sugars, and ultra processed foods. It’s not a short term cleanse. It’s a long-term direction.
The distinction between acute and chronic inflammation matters here. Acute inflammation is the redness around a cut it appears, does its job, and resolves. Chronic inflammation is different. It’s low grade, persistent, and often invisible. It doesn’t hurt in a clear way. It quietly contributes to cardiovascular disease, type 2 diabetes, and cognitive decline over years.
According to a 2023 review in StatPearls (NIH), consistent evidence links anti inflammatory eating patterns to lower risk, morbidity, and mortality from cardiovascular disease, type 2 diabetes, and certain cancers. The chronic inflammatory state is a significant driver and diet is one of the most modifiable levers available.
Or maybe I should say it this way: your body is stuck running a mild background alarm. The anti inflammation diet is about turning that alarm down consistently, through food, over weeks.
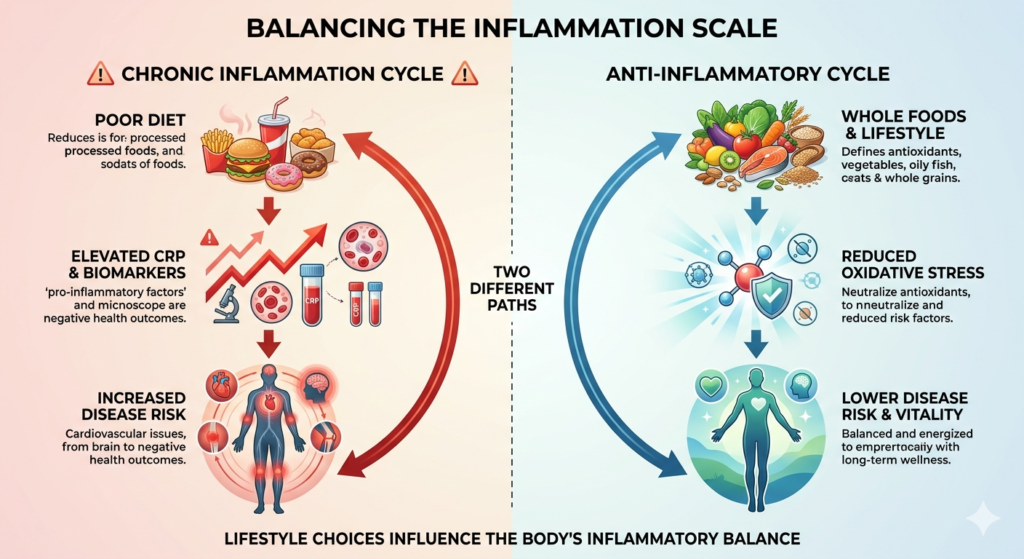
The Foods That Actually Fight Inflammation
Research consistently identifies several food categories as powerfully anti inflammatory: fatty fish, leafy greens, berries, extra virgin olive oil, nuts, legumes, whole grains, and certain herbs and spices.
A 2024 Ohio State University study published in Public Health Nutrition found that only about 34% of Americans currently follow an anti inflammatory dietary pattern. That means roughly two thirds of the people reading this are starting from a pro inflammatory baseline which is actually good news, because it means there’s meaningful ground to gain quickly.
The core anti inflammatory foods:
- Fatty fish salmon, sardines, mackerel. Aim for 2–3 servings per week. These deliver EPA and DHA omega 3 fatty acids, the best researched anti inflammatory compounds in food.
- Leafy greens spinach, kale, arugula, Swiss chard. High in polyphenols and vitamin K. Daily, in any quantity.
- Berries blueberries, strawberries, tart cherries. Anthocyanins reduce oxidative stress and suppress inflammatory cytokine production.
- Extra virgin olive oil California Olive Ranch is a widely cited brand for authentic polyphenol content; look for a harvest date on the label, not just a “best by” date. Cold pressed, unfiltered versions retain the most oleocanthal.
- Walnuts and flaxseed ALA omega 3s plus fiber. A handful of walnuts daily has shown measurable effects on CRP levels in clinical trials.
- Legumes lentils, chickpeas, black beans. Soluble fiber feeds anti inflammatory gut bacteria.
- Whole grains oats, quinoa, brown rice. Associated with lower C reactive protein (CRP), a primary marker of systemic inflammation.
- Turmeric and ginger curcumin and gingerol are among the most studied anti inflammatory plant compounds. Turmeric without black pepper (piperine) absorbs poorly. Most people taking turmeric supplements don’t know this.
A word on olive oil most people assume high fat equals inflammatory. The data says otherwise. Extra virgin olive oil’s oleocanthal compound inhibits the same COX enzymes that ibuprofen does, at a biochemical level. That’s a genuinely counter intuitive finding most food guides quietly skip over.
Quick Comparison: Anti-Inflammatory Diet Patterns
| Pattern | Best For | Key Benefit | Limitation |
|---|---|---|---|
| Mediterranean Diet | Long term heart and joint health | Most research backed; flexible and sustainable | Doesn’t restrict nightshades, which affect some autoimmune cases |
| DASH Diet | High blood pressure + inflammation | Structured, easy to follow | Lower in healthy fats; de emphasizes olive oil and fatty fish |
| Whole30 | Identifying personal trigger foods | Eliminates all common inflammatory foods | 30 day restriction; not designed for long term maintenance |
| Generic “Clean Eating” | General wellness entry point | Low barrier to start | No guidance on inflammatory markers specifically |
Mediterranean diet vs. DASH diet for inflammation: Mediterranean is better suited for reducing systemic inflammation because of its emphasis on olive oil, fatty fish, and polyphenols. DASH works better when blood pressure is the primary concern. The key difference is dietary fat quality.
The Mediterranean pattern has the strongest direct evidence for systemic inflammation reduction. That’s the model FitnoraWell’s framework is based on.
Foods That Keep Inflammation High
Most people know the obvious offenders. The less obvious ones are where compliance breaks down.
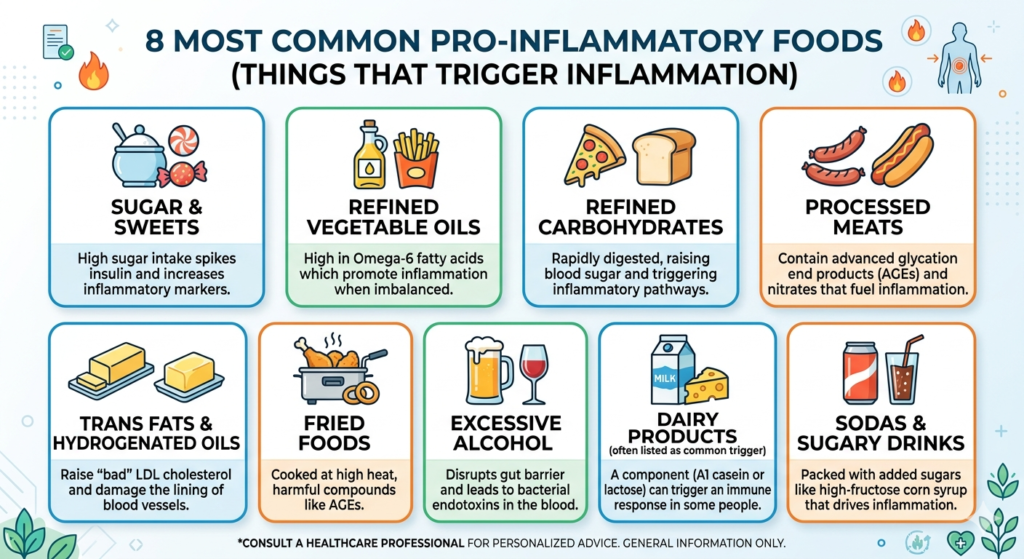
The main pro inflammatory foods to reduce:
-
Ultra processed packaged foods
microwave dinners, flavored yogurts, packaged sauces, most cereals. A 2025 report in the journal Nutrients found these foods alter gut bacteria, damage the gut lining, and switch on inflammatory gene expression in cells.
-
Added sugars
including “healthy” versions like agave and fruit juice sweetened products. Flavored protein bars, pre made smoothies, and store bought granola are common sources people don’t account for.
-
Refined grains
white bread, white pasta, white rice. These drive blood sugar spikes that directly activate inflammatory pathways.
-
Refined seed oils in excess
processed soybean, corn, and sunflower oil create an imbalanced omega 6 to omega 3 ratio, which promotes a pro inflammatory state at scale.
-
Processed and cured meats
deli meats, hot dogs, bacon.
-
Margarine and shortening
even small amounts of trans fats remain clear inflammatory triggers.
Quick note: sugar substitutes aren’t a free pass. Aspartame and erythritol may promote inflammation in some research contexts. Stevia and monk fruit appear to be the safer alternatives but even those are best used minimally, and they don’t redeem a product that’s otherwise ultra processed.
Some nutrition experts argue that dairy is universally inflammatory. That’s valid for people with a diagnosed lactose intolerance or specific immune sensitivity. But if you’re dealing with general chronic inflammation without a dairy related diagnosis, plain low fat dairy in moderate amounts doesn’t have strong evidence against it. The real culprits are ice cream, processed cheese, and flavored dairy products not plain Greek yogurt. That’s a meaningful distinction most blanket dairy warnings skip.
How Long Until You Actually Feel a Difference?
This is the question competitors never answer. It’s also the one that determines whether people stay with it.
People who’ve shifted to this eating pattern consistently report noticing reduced bloating and improved energy within 7–14 days. Measurable reductions in CRP levels typically take 4–8 weeks of consistent eating. Joint pain and skin changes which are tied to deeper immune modulation and gut microbiome shifts generally show up after 6–12 weeks.
Look if you’ve tried eating better for two weeks and felt nothing, that doesn’t mean it failed. Two weeks is barely enough time to meaningfully shift your gut microbiome composition, let alone your systemic inflammatory load. The timeline expectation was wrong, not the approach.
I’ve seen conflicting data here some studies show meaningful CRP reductions in three weeks for people starting from very high baselines; others show no statistically significant change before week eight. My read: commit to eight weeks before evaluating results. Two weeks tells you almost nothing about the deeper mechanisms.
Your First 7 Days: A Simple Starter Framework
You don’t need a rigid meal plan.
To start an anti inflammation diet this week:
- Swap your breakfast refined grain for a whole grain (oats instead of cereal, quinoa bowl instead of white toast)
- Add one fatty fish meal this week canned sardines count and cost less than $2
- Replace your cooking oil with extra virgin olive oil for all home cooking
- Add one handful of berries or one cup of leafy greens to one meal per day
- Identify one ultra processed item you eat daily and replace it with a whole food alternative
Stack all five by Day 7. That’s the entire first week job.
Day by day breakdown:
Days 1–2 Pantry audit. Remove refined oils and packaged snack foods. Stock: California Olive Ranch EVOO, canned wild salmon or sardines, a bag of green or red lentils, oats, walnuts, frozen blueberries, a dark leafy green. Thrive Market stocks most of these 20–30% cheaper than standard grocery retail worth bookmarking before your next shop.
Days 3–4 Anti inflammatory breakfast. Overnight oats with frozen blueberries, a tablespoon of ground flaxseed, and a handful of walnuts. That’s it. Done in five minutes, covers omega 3s, fiber, and polyphenols in the same bowl.
Days 5–6 Anti-inflammatory dinner. Baked salmon with roasted broccoli and quinoa. This single meal covers EPA/DHA, fiber, polyphenols, and whole grain carbohydrates. If you’re buying canned sardines instead, mix them into a lentil salad with olive oil, lemon, and parsley.
Day 7 The anti inflammatory plate formula. Half the plate: vegetables or fruit. One quarter: protein (fish, legumes, or poultry). One quarter: whole grain. Fat source: olive oil. Follow this template once. See how it feels. Repeat.
You don’t need a supplement stack to start. If you’re dealing specifically with joint inflammation, JUST Ingredients Turmeric (with added piperine) is worth considering alongside dietary changes but it supports the diet; it doesn’t substitute for it.
Condition Specific Notes: Joint Pain, Bloating, and Skin
The anti inflammation diet benefits people differently depending on the condition driving their inflammation. For joint pain, omega 3 fatty acids and polyphenols are the primary levers fatty fish, walnuts, and olive oil have the strongest clinical backing. For gut driven bloating and inflammation, fiber diversity matters most. For inflammatory skin conditions like acne or eczema, reducing added sugar and refined carbohydrates shows the most direct dietary link.
Joint pain: Prioritize EPA/DHA intake above everything else. Two to three fatty fish meals per week, or a supplement like JUST Ingredients Turmeric with piperine. The curcumin without the piperine won’t absorb meaningfully this is a detail most supplement labels don’t mention clearly.
Gut inflammation and bloating: Aim for 30 different plant foods per week. That number sounds large until you realize it includes every individual vegetable, fruit, legume, nut, seed, herb, and spice. A single mixed salad with spinach, cucumber, tomato, walnuts, and hemp seeds already counts as five.
Skin: The refined carbohydrate to skin link is probably the most direct of the three. Insulin spikes from white bread, pasta, and added sugar increase sebum production and activate cytokine mediated inflammation in skin cells. People who’ve cut refined carbohydrates specifically not all carbs, just refined ones often report visible skin changes within 4–6 weeks.